Petechial rash (in up to 50% of patients).Altered mental status (e.g., confusion, lethargy or restlessness, coma).Neurological symptoms (in up to 80% of patients).Respiratory distress (in up to 95% of patients).Classic triad: Components typically develop sequentially.Symptoms develop within 12–72 hours of the inciting event. Distention of thrombi-occluded capillaries → ↑ intracapillary pressure → extravasation of RBCs into the skin → petechial rash.Dermatologic and neurological manifestations (see “Clinical features”): The exact mechanism is unknown but may be due to paradoxical embolisms or biochemical factors (e.g., systemic cytokine release).Lipases metabolize the lodged fat cells (in pulmonary arterioles) → release of free fatty acids → pulmonary arteriolar endothelial injury → acute lung injury/ respiratory distress.Nontraumatic fat embolism: ↑ cytokine levels (e.g., CRP, TNF) → agglutination of chylomicrons in the circulation → fat emboli formation.Traumatic fat embolism: fat cells from bone marrow enter systemic circulation and occlude the pulmonary arterioles → right heart failure and pulmonary edema.Others: pancreatitis, osteomyelitis, parenteral lipid infusionĮarly operative fixation is recommended in patients with long bone fractures to reduce the risk of fat embolism syndrome.Most commonly long bone fractures (e.g., femoral fracture ).Management of cardiac arrest in pregnancyīoth arterial air embolism and venous air embolism can be caused by laparoscopic surgery, cardiac and vascular surgery, endoscopic procedures, ECMO, and diving-related injuries.įat embolism, air embolism, and AFE are all clinical diagnoses.Ī potentially life-threatening condition caused by the entry of fat cells, usually from bone marrow, into the circulatory system Etiology.Arterial line: Stop flush and open the rotating hemostatic valve.Place the patient in the supine position.Consider right heart air aspiration through CVC.PIV line: Drop infusion source below heart level.Apply an occlusive dressing to open wounds or catheter sites.Place the patient in the left lateral decubitus position and Trendelenburg position.RV dysfunction followed by severe LV dysfunction on echocardiography.Fetal debris, cells, and/or hair in pulmonary artery sample.Air bubbles in retinal vessels on fundoscopy.Signs of systemic organ ischemia on imaging (e.g., stroke neuroimaging).Air in left heart chambers on echocardiography.Air in right heart chambers and pulmonary circulation on imaging and echocardiography.Bilateral patchy infiltrates on chest imaging.Clinical features of retinal vessel occlusion.Clinical features of acute coronary syndrome. 
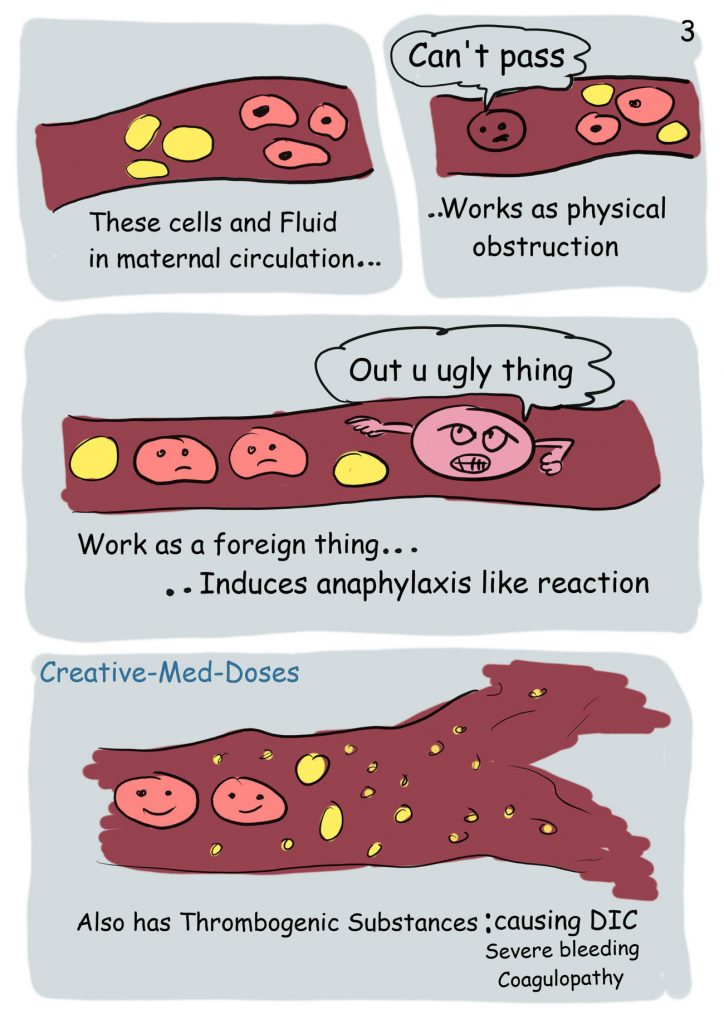
Clinical features of stroke by affected vessel.Trauma or intentional injury to arteries.Fetal cells and debris from amniotic fluid in the maternal circulation.Nonthrombotic embolisms have a high mortality rate.įor thromboembolic diseases, see “ Pulmonary embolism,” “ Thromboembolic stroke,” “ Acute mesenteric artery embolism,” “ Acute limb ischemia,” and “ Retinal vessel occlusion.” Management is mainly supportive and includes oxygenation, mechanical ventilation, and, if necessary, administration of vasopressors. Nonthrombotic embolisms are primarily a clinical diagnosis, but results of arterial blood gas analysis, ECG, and chest imaging (e.g., chest x-ray, CT) can support the diagnosis and rule out alternative causes. Characteristic clinical findings include a nondependent petechial rash on the upper body in fat embolism, the mill wheel sign in venous air embolism, signs of stroke in arterial air embolism, and disseminated intravascular coagulation in amniotic fluid embolism. General clinical features of nonthrombotic embolisms include acute onset of hypoxia, hypotension, and neurological symptoms (e.g., altered mental status, seizures). The emboli usually lodge within the pulmonary arteries and cause right ventricular outflow obstruction and circulatory collapse. Air can enter the circulatory system as a result of invasive procedures (e.g., vascular surgery or catheterization, neurological surgery), trauma, or rapid ascent when diving ( decompression illness), while amniotic fluid emboli typically occur during labor. Fat emboli mostly originate from the bone marrow in patients with long bone fractures. The blockage of blood vessels by fat, air, or amniotic fluid is an uncommon but potentially life-threatening event. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
